It's not a term you might've heard but it's a disturbance you've very likely experienced. What is parasomnia – the daunting name describing something that keeps you from sleeping peacefully?
Experiencing sleep disorders can be extremely daunting. It can be hard to figure out what causes them — and, in turn, how to recover from them. The worst part is that the anxiety of having a sleeping disorder can just make the symptoms worse. A lot of them fall under the same umbrella term of parasomnia.
So what is parasomnia exactly? What are its symptoms? Well, that’s where it gets tricky — there are several parasomnia types that can occur at various stages of sleep and are very different from each other.
Today, we’ll be answering the question “what is parasomnia?” and look into the REM and NREM parasomnias. We’ll discuss what symptoms are common for each disorder and what the leading causes for them can be.
Finally, we’ll see what we can do in order to recover from parasomnia and return to normal, blissful sleep. We’ll look at a range of personal changes those suffering from sleep disorders can make — from attending therapy to upgrading their sleep gear.
Table of Contents
- 1. What Is Parasomnia?
- 1.1. NREM Parasomnias
- 1.2. REM Parasomnias
- 1.3. Other parasomnias
- 2. Parasomnia Treatments
- 2.1. Therapy
- 2.2. Medical Treatment
- 2.3. Reducing Stress
- 2.4. Sleep Hygiene
- 3. Improving Your Sleep Environment
- 3.1. Saatva — The Leading Name in the Market
- 3.2. Puffy — A Relaxing Solution for Your Muscles
- 3.3. Layla — The 2-in-1 Comfort and Quality
- 4. Summary
- 5. Conclusion
What Is Parasomnia?
To start off, we need to answer the key question — what is parasomnia?
Parasomnia is a group of sleep disorders. They present themselves through unwanted physical behaviors during particular stages of sleep. They are usually defined by whether they happen during the REM (rapid eye movement) or NREM (non-rapid eye movement) phases of sleep.
Parasomnia is particularly common in children. However, adults can also suffer from some of the parasomnia symptoms.

As we look into the specific parasomnia examples, we will establish how they’re grouped, as well as explain what REM and NREM sleep phases are, according to the International Classification of Sleep Disorders-3 (ICSD-3).
There are numerous conditions classified as parasomnia[1], and it’s not possible to cover all of them in-depth in this article. However, understanding how some of the REM, NREM, and miscellaneous parasomnia types differ can help you answer the question of what is parasomnia.
NREM Parasomnias
NREM, also known as non-rapid eye movement, is an early sleep phase. An uninterrupted NREM phase can last about 90 minutes to two hours. It consists of three stages:
- N1 — the earliest stage. It happens right after falling asleep. It’s defined as light sleep that lasts for about 10 minutes
- N2 — the middle stage. It lasts about 30-60 minutes. During this stage, the body muscles relax a little
- N3 — the final, deep sleep stage. It lasts about 20-40 minutes. This is where brain activity increases and the sleeping body might start moving. The N3 stage transitions into REM sleep
We spend the majority of our time asleep in the NREM phase. Since the muscles don't tense up during this stage[2], it's more likely for people to move abnormally or even start walking.

Here are some of the NREM parasomnias:
- Confusional Arousals
Have you ever woken up feeling completely disoriented? Kind of drunk? Then you’ve probably experienced confusional arousal, also known as sleep drunkenness. This is a type of NREM parasomnia that happens around the third stage of sleep.
A person experiencing confusional arousal may temporarily struggle with recognizing their environment. They might feel confused, have difficulty talking, their movements might be slow. It can take anywhere from a few minutes to a few hours for them to snap back.
This condition is a lot more common in children[3]. However, it’s not unusual for adults under the influence of alcohol or drugs to experience sleep drunkenness.
- Sleepwalking
Somnambulism, or sleepwalking as it’s more commonly known, is considered by some to be one of the creepiest sleeping disorders. People experiencing it move without any cognitive awareness. It happens during the third stage of NREM sleep. It's one of the most common examples online when you search up what is parasomnia.
A sleepwalker’s actions can vary from simply walking with eyes open to playing musical instruments or even leaving the house. This condition can lead to life-threatening unconscious behavior.
There are numerous causes for sleepwalking. Some are related to mental health, especially anxiety. Others could be the influence of medication or physical injuries. Since the causes are unique to each case, it can be hard to design a treatment plan.

- Sleep Terrors
You might also know them as night terrors. Although they’re often thought of as just nightmares, there’s an important distinction between the two. People suffering from sleep terrors have an intense physical reaction. They may scream or cry.
Both adults and children may suffer from sleep terrors. However, children make up the better part of this demographic. It can sometimes be mistaken for what is parasomnia-affected REM dreaming, or a nightmare disorder.
Sleep terrors are closely tied to traumatic experiences[4]. This type of NREM parasomnia can also be tied to sleep anxiety and other adjacent health issues. If it persists, it can affect both mental and physical health.
- Sleep-Related Eating Disorders
This is a type of eating disorder where the suffering person binge eats while partially awake. People who deal with parasomnia symptoms like involuntary binge eating in the NREM phase[5] can experience weight gain, dental issues, and even injuries while handling food.
Diagnosing sleep-related eating disorders is complicated[6]. It can be hard to differentiate between what is parasomnia-induced binge eating and what is disordered eating around bedtime.
Sleep-related eating disorders can be tied to other medical conditions, like autoimmune diseases. They may also be caused by medication or substance abuse, or be closely tied to other eating disorders.
Latest Saatva Coupon Found:
UP TO $500 OFF
Limited-time Saatva Sale
We're sharing a limited-time Saatva mattress discount with our readers! Grab this deal & enjoy your new mattress with huge discounts.
REM Parasomnias
REM, or rapid eye movement, is the deep sleep phase. This is when people may experience dreaming. This stage lasts around 90 minutes and the brain reaches peak activity.
During a sleep period, you rotate between the NREM and REM phases several times. Getting enough REM sleep is essential for feeling healthy and rested. The amount of REM sleep you need changes over time. However, for adults, spending 20-25% of total sleep time in the REM stage is optimal.

What is parasomnia during the REM phase distinguished by? Usually, the sleeper may remember that the sleep disturbance occurred. For example, they may feel lingering physical discomfort or recall unpleasant dreams.
Some common REM parasomnia examples are:
- REM Sleep Behavior Disorder
REM sleep behavior disorders, RBDs for short, manifest when the sleeper reenacts their dream behavior[7]. In some cases, this can look similar to night terrors as it involves physical and vocal reactions. However, it happens in the REM sleep state.
RBD can often point towards deeper physical or neurological issues[8]. It has been linked to multiple sclerosis and narcolepsy, among other conditions. Some studies have also found a link between RBD and consuming too much coffee and chocolate.
- Sleep Paralysis
Sleep paralysis is a type of parasomnia that renders the sleeper unable to move their muscles. This takes place in the REM sleep state and is a reaction to the intensified brain activity.
A body reaction known as muscle atonia happens during the REM phase. This is a temporary paralysis of the muscles. If this reaction is prolonged, it can turn into a benign condition. Sleep paralysis is often linked to other sleep disturbances[9], like sleep deprivation or jet lag.

- Nightmare Disorder
Nightmares and sleep terrors are often falsely assumed to be one and the same. But that’s not the case for these two parasomnia examples. For starters, sleep terrors happen in the NREM phase, while nightmares occur in the REM phase, when we experience dreams.
It’s as hard to determine the cause for nightmares as it is to understand why we dream at all. It can be tied to multiple factors, from trauma and stress to illness and medication.
Nightmares are common in all age groups[10]. They are not always chronic. In fact, may only be a one-time occurrence. This makes them one of the trickiest parasomnia types to treat.
- Exploding Head Syndrome
Exploding head syndrome is a specific type of hallucinations. It affects a small number of the population and tends to affect women more.
Don’t worry — it doesn’t mean your head literally explodes. It describes a particularly weird kind of parasomnia. The sufferer is woken up by a sudden explosive noise that happens inside their head.
The exploding head syndrome may be a sign of developing neurological disorders. It may point towards epilepsy or hearing issues. People experiencing it are often able to treat the symptoms with medication.

- Hallucinations
There are two types of sleep hallucinations – hypnagogic and hypnopompic[11]. Hypnagogic hallucinations happen just before entering deep sleep and can occur alongside sleep paralysis. Meanwhile, hypnopompic hallucinations take place while waking up.
When sleep hallucinations occur, the sleeper’s five senses – taste, touch, smell, sight and hearing – are tricked into thinking that something in a dream is real[12]. It gets hard to tell the dream and reality apart. This can cause distress and even fear upon waking up.
There are many causes for sleep hallucinations. Some of the most common causes are stress and anxiety. It can be closely tied to other parasomnia types and sleep disorders. Alcohol and drug use can also trigger hallucinations.
- Sleep Enuresis
Sleep enuresis is the scientific name for bedwetting. It’s an involuntary body reaction during sleep. It can be caused by genetic issues, various illnesses or a small bladder.
Sleep enuresis is a lot more common among children over the age of five[13]. It tends to become less frequent and completely disappear with age. However, it can also be experienced by adults.

Did you know?
Have you ever wondered which mattresses are approved as the best for sleep?
See & compare TOP mattresses side by sideOther parasomnias
What is parasomnia is not necessarily defined by when it occurs. The most important aspect is the physicality of sleep behavior. Some parasomnia types are classified outside the REM and NREM phases as they happen regardless of the sleep phase.
- Sexsomnia
Sexsomnia describes various involuntary sexual activities done while asleep. While it can be caused by medications, it’s been reported that it’s common among sleepers suffering from Parkinson’s disease[14].
- Somniloquy
Sleep-talking happens during the stage between sleeping and waking. It can vary from simple sounds to complete sentences or even holding conversations[15]. It’s usually caused by other sleep disorders, stress or fever-inducing illnesses.
- Leg Cramps
Leg cramps can occur when the muscles suddenly cramp up while sleeping. While they can be related to physical activity or dehydration, there’s no single clear cause for them.

- Restless Leg Syndrome
Restless leg syndrome (RLS) is different from leg cramps. It’s described as an uncontrollable urge to move your legs. It’s very common in children and happens right before sleep. It’s been noted that treatment of RLS helps improve other parasomnia symptoms[16].
- Cardiac Arrhythmia
Cardiac arrhythmia, or irregular heart rhythm, to make it simpler, is common among parasomnia sufferers with cardiovascular diseases. REM parasomnias typically cause bradycardia, an abnormally slow heart rate. Medical treatment alongside CPAP machines can help manage the symptoms.
- Bruxism
Bruxism, commonly known as teeth grinding, is a condition that can lead to serious long-term teeth damage. Children tend to suffer from it as their baby teeth and early adult teeth grow. Bruxism in adults is often caused by stress and tension.
Parasomnia Treatments
Answering the “what is parasomnia” question may lead to even more questions than answers. With so many different parasomnia examples that tend to overlap, how do you find the right treatment?
There are different approaches to treating the most prominent parasomnia symptoms. While in some cases changing your sleep environment may be enough, sometimes medical intervention is necessary.

Here are some of the recommended treatments for NREM and REM parasomnias.
Therapy
Two of the most common causes of various parasomnias are stress and anxiety. If a person is experiencing anxiety spikes or psychological trauma, it may affect not only their mental health when they’re awake but also as they sleep. These conditions can be debilitating.
It’s not always easy to try to manage parasomnia symptoms on your own. Sometimes it might cause even more stress – and make the symptoms worse. If you feel like your mental health may be negatively affecting your sleep, it could be a good idea to get in touch with a therapist.
While therapy may not be the end-all-be-all cure for parasomnia, it can help you learn how to manage your anxiety levels and develop healthier thinking patterns.

It’s not just talking for the sake of talking, either. Some evidence suggests that cognitive-behavioral therapy (CBT) can be helpful in treating various parasomnia symptoms.
Some of the parasomnia symptoms, like night terrors and nightmares, can be tied to traumatic experiences. In these cases, Eye Movement Desensitization and Reprocessing (EMDR) therapy may be used. It’s an intensive theory set to help manage symptoms of PTSD.
Another therapeutic method that was proven to be effective in treating NREM parasomnias, as well as general stress, is Mindfulness-Based Stress Reduction (MBSR).
MBSR is used to help manage intrusive thoughts and reduce stress levels. Practicing MBSR regularly alongside medication helps alleviate stress-based parasomnia symptoms.

As both NREM and REM parasomnias can be caused by substance abuse, it may be useful to look into addiction resources and, in some cases, even in-patient treatment. Proper addiction management would require professional help to reduce the risk of relapse.
Counselors can help both children and their parents when it comes to parasomnia management. Since not all children can communicate what causes them distress and sleep problems, a child therapist can help the parents find the right strategy to manage the condition.
Medical Treatment
In some cases, therapy may not be sufficient as a treatment for parasomnia symptoms. In this case, medical intervention may be required.
Usually, this means receiving medication or sleep supplements. In any case, a consultation with a doctor may help find the medical cause of a sleep disorder.

What is parasomnia caused by in your particular case? Depending on the type and severity you’re experiencing, you may need professional help to determine the root cause.
Patients suffering from parasomnias may be examined using a polysomnogram or an electroencephalogram (EEG). These tools are used in a sleep study that monitors brain activity, breathing, and heart rate during sleep.
Polysomnograms help determine if you’re experiencing parasomnia, and if so, what can be done to treat it.
Sometimes, parasomnia might point towards a different neurological or genetic condition. For example, REM sleep behavior disorder might point towards early-onset dementia. This can help get started on the treatment years before it fully sets in.

For parasomnias caused by mental illnesses, patients may be prescribed antidepressants, anti-anxiety medication, or similar treatment. They can help restore the chemical imbalance in the brain and improve sleep quality.
According to research, melatonin has been an effective strategy in treating some types of parasomnia. However, melatonin use should be carefully adjusted by a medical professional as its dosage is unique to each user and can pose a risk of overdosing.
Parents of young children should consult a pediatrician if they see any signs of parasomnia symptoms. Usually, children do not require medical intervention because they experience changes in sleep patterns as they grow. However, a pediatrician may advise how to adjust sleep hygiene to reduce the symptoms until they fully disappear.

Some medications should not be taken alongside alcohol and other substances. This may aggravate the symptoms of parasomnia. Patients should consult a medical professional to find out if it may be unsafe.
It’s important to note that sleep disorders should not be self-medicated. It’s crucial to discuss them with your GP or a neurologist before starting any medical treatment.
It should also be emphasized that some medical treatments can cause parasomnias as a side effect. If these side effects occur, you should contact your doctor to discuss alternative options.
Reducing Stress
Yes. Easier said than done. However, it can help immensely with managing a sleep disorder. While therapy and medication are sometimes necessary, there are steps you can take in your daily routine to make parasomnia more manageable.

As of writing this article, the world is still going through the COVID-19 pandemic. It’s a stressful time for many people, and has even led to specific sleep issues related to the pandemic. Stress levels are high, and there’s still plenty of uncertainty. Stress management isn’t easy.
Of course, you don’t need to turn your life upside down in a day. You can start with small steps and work your way up until you notice improvements.
Ask yourself: what is parasomnia making the hardest for you? What adjustments can you make to make life simpler for you and the symptoms at the very least more manageable?

Caffeine can be a serious stress trigger. It stimulates your brain and may leave you antsy and restless once it’s finally bedtime. Instead of yet another cup of coffee or black tea, you may instead opt for a cup of herbal tea that will help you fall into a calm sleep.
You can also try aromatherapy. While this is by no means a replacement for medical treatment and should not be used as self-medication, certain scents can trigger your brain and help you relax.
Mindfulness, yoga, and meditation can help you manage your stress levels as well as sleep better. Breathing exercises will help you keep your heart rate steady and destress before bedtime.
Sleep Hygiene
It’s worth considering changing not only your daytime habits but your nighttime routine, too. Where you sleep can have a massive impact on how you sleep.

One of the most important steps in managing your sleep properly is setting a healthy sleep schedule. While this can take time, there are some strategies to help you fall asleep faster and easier.
Start by trying to go to bed earlier each night until you train yourself into falling asleep at the most optimal time. The amount of sleep you need depends on your age. However, it can also depend on your hormonal balance, melatonin levels, and genetics, among other factors.
Try changing your sleep position. According to research, sleeping on your back can make you more prone to sleep paralysis. The way you sleep may be impacting not only your physical health, but your sleep quality as well. Don’t be scared to switch things up.

As comfortable as it can be, don’t work where you sleep. Your bed should essentially be for sleep and sex only. Other activities will disrupt your brain and break the bed=sleep link that it’s formed.
Improving Your Sleep Environment
One of the biggest things you can do to improve the quality of your sleep hygiene is to make sure your bed is comfortable and fits your physical and medical needs.
Your bed is a significant factor in your overall sleep quality. Since certain parasomnia types are tied to physical conditions, it’s important that your sleep environment suits your needs and doesn’t cause even more discomfort.

If your parasomnia symptoms are worsened by a physical condition, it might be time to change not only how but also where you sleep. It’s possible that your mattress is either too soft or too hard for you. Perhaps it’s simply too old and can’t provide the support you need anymore.
Of course, a mattress is not exactly something you'd call a frequent purchase. It can be hard to know where to start looking and what features to keep in mind. However, when it comes to excellent quality and affordable prices, there are three obvious choices – Saatva, Puffy and Layla.
Saatva — The Leading Name in the Market
Saatva is one of the best-known names in the industry. And that’s not without reason. It’s one of the market leaders when it comes to all things sleep – from mattresses and pillows to bed sheets and even weighted blankets.

Saatva stands out for its unique mattress structure. Its Classic mattress is innerspring, yet thanks to its structure, it suppresses noise really well. This can help you sleep more soundly and with fewer distractions.
One of the most important aspects for people suffering from various parasomnias may be edge support. Those suffering from night terrors, sleepwalking or restless leg syndrome may sleep more comfortably and reduce the risk of injuring themselves thanks to the product’s solid edge support.
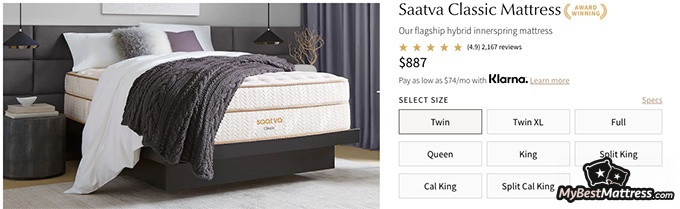
Saatva mattresses also maintain great temperature neutrality and breathability. If you’re sleeping with a fever, it may help you stay relatively cool and experience fewer sleep disturbances.
Whether it’s mattresses or the rest of the sleep range, the Saatva brand name guarantees excellent quality, eco-friendly products, and years of reliable service. Saatva is certainly one of the top choices to aid you in your parasomnia recovery.
Puffy — A Relaxing Solution for Your Muscles
Puffy is known for its foam mattresses and support for all sleeper types. These mattresses are silent, comfortable, and adjustable no matter how much of a fussy sleeper you are. It offers excellent quality for an affordable price and is ideally suited for couples.
If you’re experiencing parasomnia and have to share a bed with someone else, they may complain about sudden movements or tossing and turning. Puffy’s excellent motion isolation will absorb your movements and allow both you and your partner to rest more comfortably.
One of Puffy’s standout qualities is its pressure point relief. Parasomnia can cause physical discomfort, tension, and even temporary paralysis. Puffy’s mattresses will adjust to your body and help you maintain your spine straight. It can help alleviate muscle pain and relax the whole body.
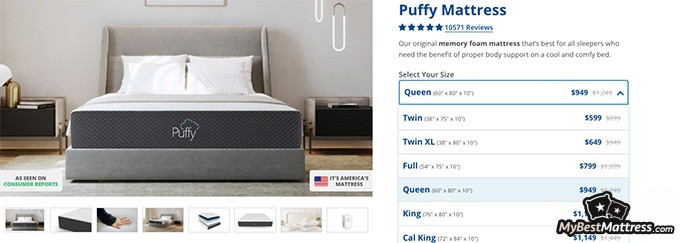
If you’re looking for comfort on a budget, Puffy is a good place to start. It’s ideal for those whose parasomnia causes them physical pain. It’ll make your partner’s sleep easier and calmer, too.
Layla — The 2-in-1 Comfort and Quality
Layla is a market name with perhaps one of the most unique products. Their copper-infused memory foam mattress has a standout feature. It’s a 2-in-1, completely flippable mattress.

As you fix your sleep habits, you may need to relearn what you thought comfortable sleeping was all about. This might mean changing the firmness of your mattress. Whether you’re used to sleeping softer or firmer, Layla has you covered.
The mattress is constructed of four inner layers. One of them, the support foam, controls the motion transfer and ensures minimal bounciness once you sleep on it. This can help reduce the risk of injury during parasomnia episodes and ensure comfort for the whole body.

The Layla 2-in-1 mattress is suitable for all sleeper types. So, if you find that one sleep position triggers your sleep problems more, you won’t have too many issues adjusting yourself.
With its adjustability and support for all sleeper types, Layla can be a great choice for those suffering from parasomnia. It provides pressure relief and full-body support without hurting your wallet.
Summary
So, what is parasomnia, according to research?
It’s a group of sleep disorders that present as involuntary physical reactions. They are separated into NREM and REM parasomnias. Parasomnias can affect sleepers of all ages; however, some disorders are more common in specific age groups.

There are numerous causes for parasomnia-type disorders. In some cases, it can be caused by substance abuse or appear as side effects of medication. In others, it can be a comorbidity of other illnesses or be related to a genetic condition. Stress and mental illness can also be triggers for these sleep disorders.
While for some sufferers parasomnia can resolve naturally – especially in children – others may require further steps to recover. Treatment methods can vary from simple life changes to consultations with neurologists.
Medical intervention can be crucial if you want to answer the question of what is parasomnia doing to your physical and mental health. Whether it’s therapy or medication, it can help you find the root cause of your sleep problems and treat them effectively.

Changes to your sleep environment can help improve your sleep quality and recover from unwanted disturbances. By upgrading your mattress, you may find that you sleep more easily and experience less physical discomfort.
Note that there may not be a single fix to some types of parasomnia. You may be required to switch the strategies around or, if you take medication, adjust it to suit your needs. You may even find that mixing and matching some of the treatment methods helps improve your sleep quality.
Conclusion
Parasomnias can be detrimental. But they’re not inevitable. There are clear steps you can take to return to restful, healthy sleep. Whether it’s trying out therapy, working with a doctor, or changing what you sleep on – all you have to do is take the first step.
And here’s the most important thing: this isn’t permanent. Sleep disturbances don’t have to be a death sentence. And while it might take some time, it’s possible to recover and go back to normal.
So, it’s time to push the sleep terrors away. Good luck, and sleep tight.
Scientific References
1. Shantanu Singh, Harleen Kaur, Shivank Singh et al. 'Parasomnias: A Comprehensive Review'
2. Anna Castelnovo, Régis Lopez, Paola Proserpio et al. 'NREM sleep parasomnias as disorders of sleep-state dissociation'
3. Gregory Stores 'Dramatic parasomnias'
4. Alexander K. C. Leung, Amy A. M. Leung, Alex H. C. Wong et al. 'Sleep Terrors: An Updated Review'
5. Giacomo Chiaro, Maria Turchese Caletti and Federica Provini 'Treatment of sleep-related eating disorder'
6. Dr. Carlos H. Schenck and Mark W. Mahowald 'Review of nocturnal sleep-related eating disorders'
7. Bradley F. Boeve 'REM Sleep Behavior Disorder: Updated Review of the Core Features, the RBD-Neurodegenerative Disease Association, Evolving Concepts, Controversies, and Future Directions'
8. Alessandra Coeytaux, Keith Wong, Ron Grunstein et al. 'REM sleep behaviour disorder: More than just a parasomnia'
9. Esther Olunu, Ruth Kimo, Esther Olufunmbi Onigbinde et al. 'Sleep Paralysis, a Medical Condition with a Diverse Cultural Interpretation'
10. Annika Gieselmann, Malik Ait Aoudia, Michelle Carr et al. 'Aetiology and treatment of nightmare disorder: State of the art and future perspectives'
11. Flavie Waters, Jan Dirk Blom, Thien Thanh Dang-Vu et al. 'What Is the Link Between Hallucinations, Dreams, and Hypnagogic–Hypnopompic Experiences?'
12. J. Allan Cheyne, Steve D. Rueffer and Ian R. Newby-Clark 'Hypnagogic and Hypnopompic Hallucinations during Sleep Paralysis: Neurological and Cultural Construction of the Night-Mare'
13. C. Carolyn Thiedke 'Nocturnal Enuresis'
14. Todd J. Swick 'Parkinson's Disease and Sleep/Wake Disturbances'
15. Isabelle Arnulf, Ginevra Uguccioni, Frederick Gay et al. 'What Does the Sleeping Brain Say? Syntax and Semantics of Sleep Talking in Healthy Subjects and in Parasomnia Patients'
16. Neepa Gurbani, Thomas J. Dye, Kyle Dougherty et al. 'Improvement of Parasomnias After Treatment of Restless Leg Syndrome/ Periodic Limb Movement Disorder in Children'
Leave your honest feedback
Leave your genuine opinion & help thousands of people to choose the best mattress. All feedback, either positive or negative, are accepted as long as they’re honest. We do not publish biased feedback or spam. So if you want to share your experience, opinion or give advice - the scene is yours!